Quick Answer: Best Bone Health building stronger bones requires a multi-pronged approach combining adequate calcium and vitamin D intake, vitamin K2 for proper calcium utilisation, regular weight-bearing exercise, and reducing habits that deplete bone density. Most adults need 700–1,200 mg of calcium daily, paired with 10–25 mcg of vitamin D, though individual needs vary—always discuss supplementation with your GP.
Strong bones form the structural foundation of your body, yet bone health often goes overlooked until problems arise. By understanding how bones grow, maintain themselves, and what nutrients they require, you can take practical steps today that support skeletal strength for decades to come—regardless of your current age.
Your skeleton is far more dynamic than most people realise. Bones constantly break down and rebuild themselves through a process called remodelling, with your entire skeleton replacing itself roughly every ten years. This means the choices you make now—what you eat, how you move, which supplements you consider—directly influence the strength and density of your bones in the years ahead.
Whether you’re in your twenties looking to maximise peak bone mass, in midlife hoping to maintain what you’ve built, or older and wanting to slow bone loss, this guide walks you through evidence-based strategies for building and preserving stronger bones. We’ll explore the key nutrients, the exercise that genuinely helps, the habits worth changing, and how to work with your healthcare provider to create a personalised approach.
For those already exploring mineral supplementation, understanding how different nutrients interact matters enormously. Our guide on iron supplements and deficiency signs explores one mineral that plays a supporting role in bone health through its involvement in collagen synthesis.

🎬 Watch: Frequently Asked Questions.
📜 Prefer reading? Scroll down for detailed explanations.
Understanding Best Bone Health and Why It Matters
Bones serve multiple functions beyond simply holding you upright. They protect vital organs, anchor muscles for movement, store minerals your body draws upon when needed, and house the marrow that produces blood cells. When bone health declines, the consequences extend far beyond an increased fracture risk.
Bone density—the amount of mineral packed into your bones—peaks somewhere between your mid-twenties and early thirties. After this point, you gradually lose more bone than you build, though the rate varies significantly based on genetics, hormones, nutrition, and physical activity. Women experience accelerated bone loss during and after menopause due to declining oestrogen levels, but men also face bone density challenges as they age.
The good news? Research consistently shows that lifestyle factors can meaningfully slow bone loss and, in some cases, even improve bone density at any age. The strategies outlined in this guide aren’t just for those already concerned about osteoporosis—they’re relevant for anyone wanting to invest in their long-term skeletal health.
Understanding your personal risk factors helps prioritise which steps matter most for you. Family history of osteoporosis, low body weight, smoking, excessive alcohol intake, certain medications (particularly long-term corticosteroids), and conditions affecting nutrient absorption all influence bone health. If several risk factors apply to you, discussing bone density testing with your GP becomes particularly worthwhile.
Step 1: Optimise Your Calcium Intake
Prioritise Calcium-Rich Foods First
Calcium forms the primary mineral component of bone tissue. Adults in the UK need approximately 700 mg daily, though some experts suggest higher intakes—around 1,000–1,200 mg—for post-menopausal women and older adults. Food sources generally provide better absorption than supplements and come packaged with other beneficial nutrients.
Dairy products remain the most concentrated and bioavailable calcium sources. A 200 ml glass of milk provides roughly 240 mg of calcium, while a small pot of yoghurt offers around 200 mg. Hard cheeses pack even more—30 g of cheddar contains approximately 220 mg. However, dairy isn’t the only option.
Plant-based calcium sources include fortified plant milks (check labels—calcium content varies significantly between brands), calcium-set tofu, kale, pak choi, broccoli, almonds, and tinned fish with edible bones like sardines and salmon. Fortified foods can be particularly valuable for those avoiding dairy, with some plant milks matching or exceeding dairy’s calcium content per serving.
If your dietary intake falls consistently short, calcium supplements may help bridge the gap. However, more isn’t necessarily better—research suggests that very high calcium intakes (above 1,500 mg daily from food and supplements combined) may not provide additional bone benefits and could potentially increase cardiovascular risk in some individuals. Speaking with your GP before starting calcium supplements helps ensure you’re taking an appropriate amount for your circumstances.
For a deeper exploration of calcium supplementation, including different forms and absorption considerations, our complete guide to calcium supplements covers what you need to know.
Step 2: Ensure Adequate Vitamin D Levels
Address the UK’s Vitamin D Challenge
Without sufficient vitamin D, your body cannot effectively absorb calcium from food—rendering even excellent calcium intake less useful for bone health. The UK government recommends all adults consider a 10 mcg (400 IU) vitamin D supplement during autumn and winter, with some groups advised to supplement year-round.
Vitamin D is unique among nutrients because your skin produces it when exposed to UVB sunlight. Unfortunately, the UK’s latitude means that from October through March, sunlight lacks sufficient UVB strength for vitamin D synthesis, regardless of how long you spend outdoors. Even during summer, factors like sunscreen use, skin pigmentation, age, and limited outdoor time can compromise production.
Food sources of vitamin D are relatively limited. Oily fish (salmon, mackerel, sardines) provide meaningful amounts, as do egg yolks and foods fortified with vitamin D (some breakfast cereals, spreads, and plant milks). However, most people struggle to meet their needs through diet alone, making supplementation practical for many.
While 10 mcg represents the minimum recommended intake, some individuals benefit from higher amounts. Those with darker skin, limited sun exposure, obesity, or malabsorption conditions may need 25–50 mcg (1,000–2,000 IU) daily to maintain adequate blood levels. Your GP can test your vitamin D status if you’re unsure whether you’re getting enough, and this test is particularly worthwhile before starting higher-dose supplementation.
Vitamin D3 (cholecalciferol) is generally preferred over D2 (ergocalciferol) for supplementation, as research suggests D3 raises and maintains blood levels more effectively. Our detailed breakdown of vitamin D benefits and sources explores the evidence behind different forms and optimal intake strategies.
Step 3: Add Vitamin K2 for Better Calcium Utilisation
Direct Calcium Where It Belongs
Vitamin K2 activates proteins that guide calcium into bones while helping prevent its accumulation in arteries and soft tissues. This “calcium-directing” function makes K2 a valuable complement to calcium and vitamin D supplementation, though research is still evolving.
Unlike vitamin K1 (found abundantly in green leafy vegetables and primarily involved in blood clotting), vitamin K2 appears to play a more direct role in bone and cardiovascular health. The body can convert some K1 to K2, but this conversion is limited and inefficient in many people.
Food sources of vitamin K2 include fermented foods (particularly natto, a Japanese fermented soybean dish that’s extremely rich in K2), certain cheeses (especially Gouda and Brie), egg yolks, and grass-fed animal products. Because natto is an acquired taste unfamiliar to most Western palates, and other food sources contain relatively modest amounts, K2 supplements have become popular.
Two main forms of K2 supplements exist: MK-4 and MK-7. MK-7 (derived from fermented foods) has a longer half-life in the body, meaning it remains active longer after a single dose. Typical supplemental doses range from 45–200 mcg daily, though optimal amounts remain under investigation.
For those taking blood-thinning medications like warfarin, vitamin K supplementation requires careful medical supervision, as vitamin K influences how these medications work. Our resource on vitamin K2 benefits for bones and heart examines the current evidence and practical considerations.
💡 Tip: Many bone health supplements now combine calcium, vitamin D3, and vitamin K2 in a single product, reflecting the synergy between these nutrients. However, quality and dosing vary considerably—check that each nutrient is present in meaningful amounts rather than just token quantities.
Step 4: Incorporate Weight-Bearing and Resistance Exercise
Stress Your Bones (In a Good Way)
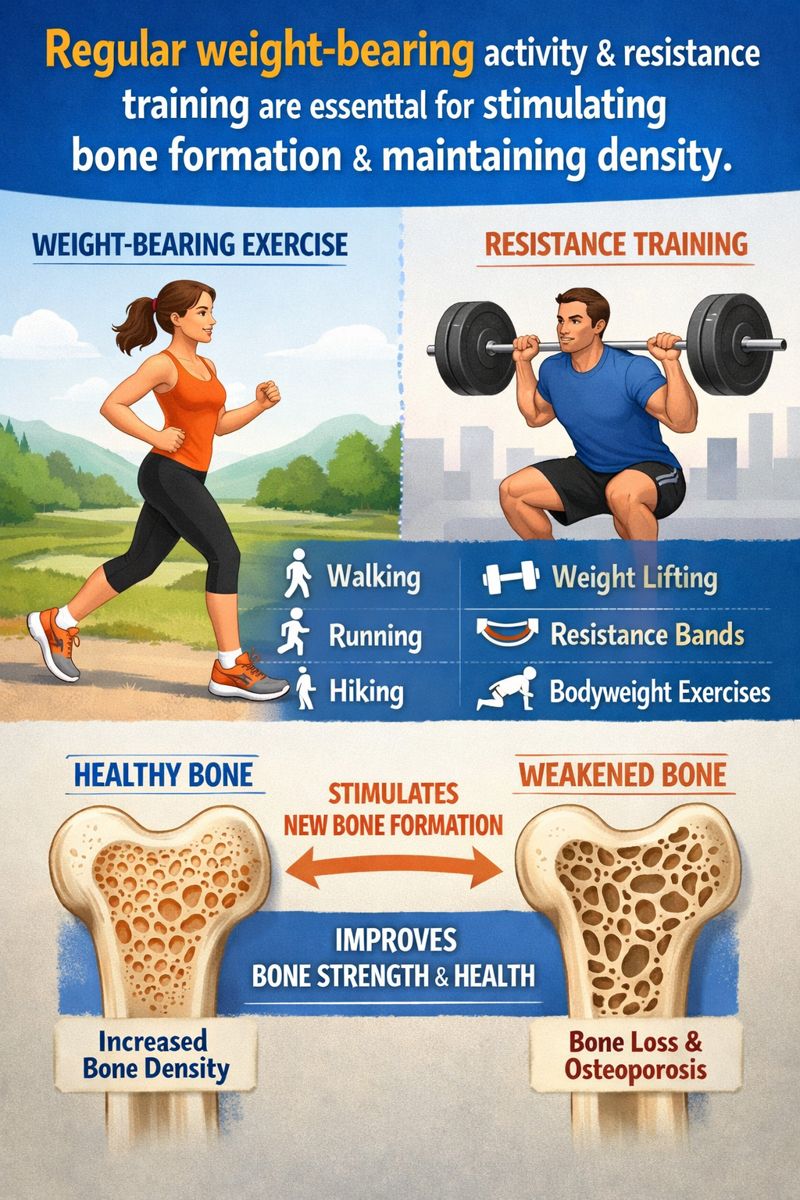
Bones respond to mechanical stress by becoming stronger—a principle called Wolff’s Law. Activities that load your skeleton stimulate bone-building cells (osteoblasts) to deposit new bone tissue, while sedentary behaviour signals your body that strong bones aren’t needed.
Weight-bearing exercises force you to work against gravity while staying upright. Walking, jogging, hiking, dancing, tennis, and climbing stairs all qualify. These activities are particularly beneficial for the hips, spine, and legs—sites especially vulnerable to osteoporotic fractures.
Resistance training (lifting weights, using resistance bands, or working against your own body weight) stimulates bone formation at the sites where muscles attach. Research suggests that higher-impact activities and heavier resistance loads provide greater bone-building stimulus than lighter, lower-impact alternatives, though any activity beats none.
Swimming and cycling, while excellent for cardiovascular fitness, don’t load the skeleton as effectively because they’re not weight-bearing. If these are your preferred activities, consider adding some weight-bearing or resistance work to your routine specifically for bone health.
Consistency matters more than intensity for most people. Aim for weight-bearing activity most days of the week and resistance training two to three times weekly, targeting major muscle groups. If you’re new to exercise or have existing health conditions, working with a physiotherapist or qualified fitness professional helps ensure you’re exercising safely and effectively.
Step 5: Reduce Bone-Depleting Habits
Identify and Address Bone-Harming Behaviours
Certain lifestyle factors actively undermine bone health, sometimes negating the benefits of good nutrition and exercise. Addressing these habits amplifies the positive effects of the steps above.
Smoking interferes with bone health through multiple mechanisms. It impairs calcium absorption, reduces oestrogen levels (which protect bones), damages blood vessels that nourish bone tissue, and may directly affect bone cells. Smokers have significantly lower bone density and higher fracture rates than non-smokers. Quitting at any age provides bone health benefits, with some recovery of bone density observed after stopping.
Excessive alcohol disrupts bone remodelling and interferes with calcium absorption. While moderate alcohol intake (within recommended guidelines) may not significantly harm bones, regular heavy drinking clearly increases osteoporosis and fracture risk. If you drink, staying within the recommended limit of 14 units per week, spread across several days, helps minimise bone-related risks.
Very high caffeine intake may modestly reduce calcium absorption, though the effect appears relatively small when calcium intake is adequate. Drinking a few cups of coffee or tea daily is unlikely to meaningfully harm bones, particularly if you consume sufficient calcium. Replacing milk with water or black coffee removes a calcium source, however, which may be more relevant than the caffeine itself.
Excessive sodium increases urinary calcium excretion. While the bone health impact of typical sodium intake remains debated, reducing very high salt consumption aligns with broader health recommendations and may offer modest bone benefits.
Prolonged sedentary behaviour signals to your body that strong bones aren’t necessary. Even if you exercise regularly, spending most of your remaining waking hours sitting may partially offset those benefits. Finding opportunities to stand, walk, and move throughout the day supports bone health beyond dedicated exercise sessions.
Step 6: Support Your Bones With Key Minerals
Consider Additional Supporting Nutrients
While calcium and vitamin D receive the most attention, several other minerals and nutrients contribute to bone health. Ensuring adequate intake supports the foundation you’re building with the previous steps.
Magnesium plays a role in converting vitamin D to its active form and influences bone crystal formation. Roughly 50–60% of the body’s magnesium resides in bones. Good sources include nuts (especially almonds and cashews), seeds, whole grains, legumes, and dark leafy greens. Many UK adults don’t meet magnesium intake recommendations, making it worth attention.
Phosphorus combines with calcium to form the mineral crystals that give bones their hardness. Deficiency is uncommon because phosphorus is widespread in the food supply—found in meat, dairy, fish, poultry, nuts, and legumes. In fact, excessive phosphorus (from heavily processed foods and fizzy drinks) relative to calcium intake may potentially be more concerning than deficiency, though evidence remains mixed.
Protein provides the collagen framework upon which minerals are deposited. Both inadequate and excessive protein intake have been linked to bone health concerns in some studies, though moderate-to-high protein intake from varied sources appears beneficial for most people, especially older adults at risk of muscle and bone loss.
Vitamin C is essential for collagen synthesis, the protein matrix of bone. Fresh fruits and vegetables provide abundant vitamin C, and deficiency is rare with a reasonably varied diet.
Our comprehensive exploration of magnesium types and benefits covers how different forms of this mineral are absorbed and used by the body, which matters if you’re considering supplementation.
| Nutrient | Daily Target (Adults) | Top Food Sources | Role in Bone Health |
|---|---|---|---|
| Calcium | 700–1,200 mg | Dairy, fortified plant milk, leafy greens, tinned fish with bones | Primary structural mineral |
| Vitamin D | 10–25 mcg | Sunlight, oily fish, fortified foods, supplements | Enables calcium absorption |
| Vitamin K2 | 45–200 mcg | Natto, aged cheese, egg yolks, grass-fed meat | Directs calcium to bones |
| Magnesium | 270–400 mg | Nuts, seeds, whole grains, dark leafy greens | Vitamin D activation, bone crystal formation |
| Protein | 0.75–1.2 g/kg body weight | Meat, fish, eggs, dairy, legumes, tofu | Collagen framework for mineralisation |
| Vitamin C | 40 mg | Citrus fruits, berries, peppers, broccoli | Collagen synthesis |
How These Nutrients Work Together
The nutrients supporting bone health don’t work in isolation—they interact in ways that can enhance or, in some cases, interfere with each other’s effectiveness. Understanding these relationships helps you optimise your approach and avoid common mistakes.
The calcium-vitamin D partnership represents the most well-established synergy in bone nutrition. Vitamin D increases the efficiency of calcium absorption in your intestines from around 10–15% (without adequate vitamin D) to 30–40%. This means that calcium supplementation without attention to vitamin D status may provide far less benefit than expected.
Vitamin K2 complements this pair by activating osteocalcin, a protein that binds calcium to the bone matrix. Some researchers suggest that supplementing calcium and vitamin D without K2 might increase calcium in the bloodstream without ensuring it reaches bones effectively, though this remains an area of ongoing investigation.
Magnesium enters the picture by participating in vitamin D metabolism—the enzymes that convert vitamin D to its active form require magnesium as a cofactor. Low magnesium status may therefore limit the benefits of vitamin D supplementation, even when vitamin D intake appears adequate.
| Combination | Synergy Type | Why It Works | Evidence Level |
|---|---|---|---|
| Calcium + Vitamin D | 🔄 Absorption | Vitamin D increases intestinal calcium absorption by 2–4 times | ⭐⭐⭐ Strong |
| Vitamin D + Vitamin K2 | 🔗 Cofactor | K2 activates proteins that direct calcium (made available by D) into bones | ⭐⭐ Moderate |
| Vitamin D + Magnesium | ⚡ Activation | Magnesium is required for enzymes that convert vitamin D to its active form | ⭐⭐ Moderate |
| Vitamin C + Collagen/Protein | 🔗 Cofactor | Vitamin C is essential for proper collagen cross-linking in bone matrix | ⭐⭐⭐ Strong |

Products Worth Considering
If dietary changes alone don’t provide sufficient nutrients for your bone health goals, supplements can help fill the gaps. The following products represent the types of formulations commonly used to support bone density, though individual needs vary—consulting your GP helps determine what’s appropriate for you.
Calcium + Vitamin D3 Complex
A foundational combination addressing the two most critical nutrients for bone health. Look for calcium citrate or calcium carbonate paired with vitamin D3 (cholecalciferol) in meaningful doses.
- Supports calcium absorption and bone mineralisation
- Convenient single-product approach to core bone nutrients
- Suitable for those with limited sun exposure or dietary calcium intake
Complete Bone Support Formula
Comprehensive bone health supplements combine calcium, vitamin D3, vitamin K2, magnesium, and sometimes additional trace minerals in one formulation. These address multiple nutritional factors simultaneously.
- Multi-nutrient approach reflecting current bone health research
- May include MK-7 form of vitamin K2 for extended activity
- Often includes magnesium to support vitamin D metabolism
Safety Considerations and Precautions
While the strategies outlined in this guide are generally safe for most adults, certain situations require extra caution or medical guidance. Bone health supplements, like all supplements, can interact with medications and aren’t appropriate for everyone.
Calcium supplements may interact with certain antibiotics (tetracyclines, fluoroquinolones), bisphosphonates used for osteoporosis treatment, thyroid medications, and some blood pressure medicines. Taking calcium at a different time of day—typically 2–4 hours apart—usually resolves these interactions. Very high calcium intake has been associated with potential cardiovascular concerns in some studies, though evidence remains debated.
Vitamin D toxicity is rare but possible with prolonged high-dose supplementation (typically above 100 mcg/4,000 IU daily for extended periods without medical supervision). Symptoms include nausea, weakness, frequent urination, and eventually kidney problems from excessive calcium absorption. Sticking to recommended doses and, if using higher amounts, doing so under GP guidance with periodic blood level monitoring, prevents problems.
Vitamin K supplements are contraindicated for those taking warfarin or similar anticoagulants, as vitamin K influences blood clotting—the very process these medications target. Even dietary vitamin K consistency matters for warfarin users. If you take blood thinners, discuss any supplement changes with your healthcare provider.
Underlying health conditions affecting calcium metabolism—including hyperparathyroidism, kidney disease, sarcoidosis, and certain cancers—require individualised guidance on calcium and vitamin D intake. High-dose supplementation in these contexts could cause harm.
| Combination | Risk Level | Interaction | Recommendation |
|---|---|---|---|
| Calcium + Iron supplements | MODERATE | Calcium may reduce iron absorption when taken together | Take at different times of day (2+ hours apart) |
| Calcium + Thyroid medication | MODERATE | Calcium interferes with levothyroxine absorption | Take thyroid medication 4 hours before calcium |
| Vitamin K2 + Warfarin | HIGH | Vitamin K affects anticoagulant medication efficacy | Consult GP before any K2 supplementation |
| High-dose Vitamin D + Kidney disease | HIGH | Risk of hypercalcaemia with impaired kidney function | Requires medical supervision and monitoring |
| Calcium + Bisphosphonates | MODERATE | Calcium reduces osteoporosis medication absorption | Take bisphosphonate first thing; calcium later in day |
⚠️ Important: If you’re taking any medications, have been diagnosed with osteoporosis or osteopenia, or have conditions affecting calcium metabolism, always discuss bone health supplementation with your GP before starting. What works for general prevention may need adjustment for treatment contexts.
Frequently Asked Questions
At what age should I start focusing on bone health?
The earlier the better, though it’s never too late to benefit. Bone mass peaks in your late twenties to early thirties, so building strong bones during childhood, adolescence, and early adulthood provides the best foundation. However, lifestyle changes and appropriate supplementation can slow bone loss and potentially improve bone density at any age. Post-menopausal women and men over 50 should pay particular attention to bone health strategies.
How long does it take to see improvements in bone density?
Bone remodelling is a slow process, and meaningful changes in bone density typically take 12–24 months to become measurable on DEXA scans. This doesn’t mean your efforts aren’t working—it simply reflects how gradually bones change. Consistency with nutrition, exercise, and supplementation over years, rather than weeks, produces the most significant long-term benefits. Your GP can advise on appropriate follow-up testing intervals.
Can I take all my bone health supplements together?
Many bone health supplements can be taken together, particularly calcium with vitamin D and K2, as these nutrients work synergistically. However, calcium should be separated from iron supplements and certain medications by at least 2 hours to avoid absorption interference. Taking calcium with food generally improves absorption (especially for calcium carbonate) and reduces the small risk of digestive upset some people experience.
Is dairy essential for bone health, or can I get enough calcium without it?
While dairy is a convenient and bioavailable calcium source, it isn’t essential. Many people maintain excellent bone health without dairy by consuming calcium-fortified plant milks (matching or exceeding dairy’s calcium content), calcium-set tofu, tinned fish with edible bones, leafy greens, almonds, and other non-dairy sources. Careful attention to total calcium intake becomes more important when avoiding dairy, and supplementation may help fill gaps.
Does coffee weaken bones?
Moderate coffee consumption (2–4 cups daily) is unlikely to meaningfully harm bone health, particularly if you consume adequate calcium. Caffeine may slightly increase urinary calcium excretion, but the effect is relatively small and easily offset by consuming milk in your coffee or ensuring sufficient calcium intake elsewhere. Very high caffeine intake combined with low calcium intake could theoretically contribute to bone loss over time, but for most coffee drinkers, this isn’t a significant concern.
Should I have my bone density tested?
Bone density testing (DEXA scan) is generally recommended for all women aged 65+ and men aged 70+, or earlier if you have risk factors such as family history of osteoporosis, previous fractures from minor falls, long-term corticosteroid use, early menopause, low body weight, smoking, or conditions affecting nutrient absorption. Discussing your individual risk factors with your GP helps determine whether and when testing makes sense for you. In the UK, DEXA scans are available on the NHS when clinically indicated.
Final Thoughts
Building and maintaining strong bones isn’t about any single magic solution—it’s the cumulative effect of consistent, evidence-based habits sustained over time. The six-step approach outlined in this guide addresses nutrition, exercise, and lifestyle factors that research consistently links to better bone outcomes.
Start where you are. If your diet currently lacks calcium-rich foods, that’s your first priority. If you’re sedentary, adding weight-bearing activity provides immediate benefit. If you’ve been supplementing calcium without vitamin D, addressing that gap may unlock more benefit from what you’re already taking. Small, sustainable changes compound over months and years.
Remember that bone health exists within your broader health context. The habits that support strong bones—nutritious eating, regular exercise, not smoking, moderate alcohol, adequate vitamin D—also benefit your heart, brain, muscles, and overall wellbeing. You’re not just investing in your skeleton; you’re investing in your quality of life decades from now.
If you have specific concerns about your bone health, risk factors for osteoporosis, or questions about supplementation, your GP is your best resource for personalised guidance. They can assess your individual situation, arrange bone density testing if appropriate, and help you create a plan tailored to your needs.
✓ Key Takeaways
- Calcium (700–1,200 mg daily) and vitamin D (10–25 mcg) form the foundation of bone health nutrition
- Vitamin K2 may help direct calcium into bones rather than soft tissues
- Weight-bearing and resistance exercise stimulates bone formation—aim for most days weekly
- Reducing smoking and excessive alcohol protects bone density
- Nutrients work synergistically—addressing multiple factors produces better results than focusing on one
- Bone changes slowly; consistency over years matters more than short-term intensity
Sources
- NHS. “Vitamins and minerals – Calcium.” NHS Choices. NHS — Bone Health and Calcium
- NIH Office of Dietary Supplements. “Calcium Fact Sheet for Health Professionals.” NIH ODS. NIH ODS — All Fact Sheets
- National Institutes of Health. “Vitamin D and Bone Health Research.” PubMed. PubMed — Vitamin D Bone Density Research
- Mayo Clinic. “Osteoporosis Prevention.” Mayo Clinic. Mayo Clinic — Osteoporosis Prevention
- Harvard T.H. Chan School of Public Health. “Calcium and Bone Health.” Harvard Health. Harvard Health — Bone Health
- Cleveland Clinic. “Building Strong Bones.” Cleveland Clinic. Cleveland Clinic — Building Stronger Bones
Written by Arsim Rama
Health Content Specialist · Last reviewed: January 2026
Affiliate Disclosure: This article may contain affiliate links. If you purchase through these links, we may earn a small commission at no extra cost to you. We only recommend products we believe in.
Medical Disclaimer: This article is for educational purposes only and does not constitute medical advice. Always consult your GP or qualified healthcare professional before making changes to your health regimen.