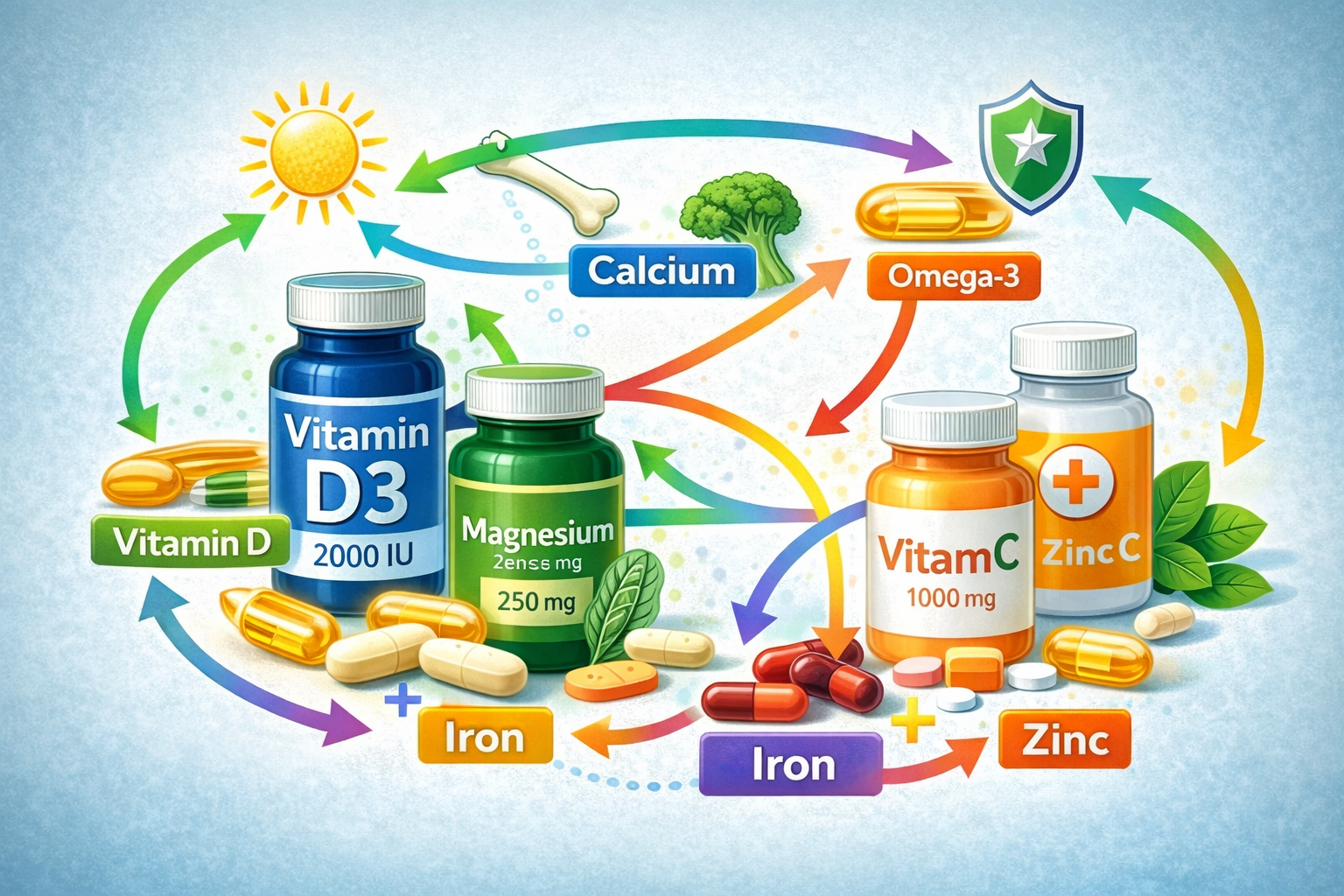
Quick Answer: Supplement interactions occur when nutrients affect each other’s absorption, effectiveness, or safety. Common examples include calcium blocking iron absorption, vitamin K interfering with blood thinners, and zinc competing with copper. Timing your supplements correctly and consulting a healthcare professional before combining multiple products may help you avoid potential problems.
Supplement interactions happen when vitamins, minerals, or herbal products affect how other substances work in your body—whether that’s another supplement, a prescription medication, or nutrients from food. Understanding these interactions matters because even beneficial nutrients can cause problems when combined incorrectly, potentially reducing effectiveness or creating unexpected side effects.
Introduction
If you take more than one supplement, you’re not alone. Surveys suggest that roughly half of UK adults use dietary supplements, with many people taking several products daily. Yet surprisingly few of us consider whether those supplements might interact with each other—or with medications we’re prescribed.
This isn’t simply an academic concern. Some interactions are relatively minor, perhaps reducing how well a nutrient absorbs. Others can be genuinely dangerous, particularly when supplements interact with prescription medications. The challenge is that supplement bottles rarely warn about these issues, and healthcare professionals don’t always have time to discuss every possible combination.
This guide aims to bridge that gap. We’ll explore the most common types of supplement interactions, explain why they happen, and offer practical strategies for timing and combining your supplements more safely. Whether you’re managing a complex supplement routine or simply wondering if your multivitamin plays nicely with your fish oil, you’ll find evidence-based guidance here.
Of course, this information doesn’t replace professional medical advice. If you take prescription medications or have underlying health conditions, speaking with your GP or pharmacist before starting any new supplement remains essential. Think of this guide as a starting point for more informed conversations with your healthcare team—and for making your own research easier. For related reading on individual nutrients, our vitamin B1 essential guide covers one important nutrient in depth.
🎬 Watch: Frequently Asked Questions.
📜 Prefer reading? Scroll down for the full written guide.
Understanding How Supplement Interactions Work
Before exploring specific interactions, it helps to understand the mechanisms involved. Supplement interactions typically fall into several categories, each working through different biological pathways.
Competition for Absorption
Many minerals use the same transport systems to cross from your gut into your bloodstream. When two competing minerals are present simultaneously, they essentially queue for the same limited number of entry points. The result? One or both may absorb less efficiently than if taken alone.
Iron and calcium represent perhaps the most well-documented example. Research suggests that taking calcium supplements alongside iron can reduce iron absorption significantly—some studies indicate reductions of 50% or more when large doses are consumed together. This doesn’t mean you can’t take both; it means timing matters.
Enhanced or Reduced Effectiveness
Some nutrients work synergistically, meaning they enhance each other’s effects. Vitamin D and calcium are a classic pairing—vitamin D helps your body absorb and use calcium more effectively. Similarly, vitamin C may enhance iron absorption from plant sources, which is why nutrition advice often suggests pairing iron-rich plant foods with citrus.
Conversely, some combinations reduce effectiveness. High doses of zinc taken over extended periods may interfere with copper absorption, potentially leading to copper deficiency if not addressed. The body’s mineral balance is interconnected in ways that aren’t always obvious.
Metabolic Interactions
Your liver processes many supplements using enzyme systems—particularly the cytochrome P450 family. When multiple substances compete for the same enzymes, or when one substance speeds up or slows down enzyme activity, the metabolism of other compounds can be affected. This mechanism is particularly relevant for herbal supplements and medications.
St John’s Wort is notorious for this. It induces certain liver enzymes, which can accelerate the breakdown of many prescription medications, potentially reducing their effectiveness. This is why it’s often flagged as a supplement requiring particular caution.
Physiological Effects
Sometimes interactions occur not through direct chemical competition but through overlapping physiological effects. Taking multiple blood-thinning supplements alongside anticoagulant medications, for instance, may increase bleeding risk—not because the substances interact chemically, but because their combined effect on blood clotting becomes excessive.
| Interaction Type | Mechanism | Example |
|---|---|---|
| Absorption Competition | Minerals compete for transport proteins | Calcium reduces iron absorption |
| Synergistic Enhancement | One nutrient improves absorption of another | Vitamin D enhances calcium uptake |
| Enzyme Induction/Inhibition | Alters liver metabolism of other substances | St John’s Wort affects drug metabolism |
| Additive Effects | Combined physiological impact exceeds safe range | Multiple blood thinners increasing bleed risk |
| Depletion | Long-term use depletes another nutrient | High-dose zinc depleting copper over time |
Common Supplement-to-Supplement Interactions
Let’s examine some of the most frequently encountered interactions between supplements themselves. These are situations where the supplements you’re taking may affect each other.
Calcium and Iron
This interaction is well-established in the research literature. Calcium appears to inhibit iron absorption through mechanisms that aren’t fully understood, though competition for transport proteins likely plays a role. The interaction seems most pronounced when both are taken together in significant amounts.
Practical solution: If you need both supplements, consider taking them at different times of day. Iron supplements are often best absorbed on an empty stomach (if tolerated), whilst calcium can be taken with meals. Separating them by at least two to four hours may help maximise absorption of both.
Calcium and Magnesium
These two minerals also compete for absorption, though the interaction may be less dramatic than with iron. Some research suggests that very high calcium intake could impair magnesium absorption, and vice versa. However, the body does have some ability to adapt to different mineral ratios over time.
For most people taking moderate supplemental doses, this interaction may not be clinically significant. That said, if you’re taking high doses of either mineral, spacing them apart might be reasonable. Magnesium supplements are often taken in the evening anyway due to their potential relaxation benefits, which naturally separates them from morning calcium.
Zinc and Copper
Zinc and copper have an inverse relationship in the body. High zinc intake stimulates the production of metallothionein, a protein that binds copper in intestinal cells and prevents its absorption. Over time, excessive zinc supplementation can lead to copper deficiency, which may cause anaemia, neurological problems, and immune dysfunction.
This typically becomes concerning at zinc doses above 40mg daily taken for extended periods. Many zinc supplements now include a small amount of copper to help maintain balance. If you’re taking zinc for specific therapeutic purposes, monitoring copper status through blood tests may be advisable.
Vitamin E and Vitamin K
High-dose vitamin E may interfere with vitamin K’s role in blood clotting. Vitamin K is essential for producing clotting factors, and vitamin E in large amounts can antagonise this process. For most people taking standard vitamin E doses, this isn’t a major concern. However, those on blood-thinning medications or with clotting disorders should be particularly cautious about vitamin E supplementation.
Omega-3 Fatty Acids and Blood-Thinning Supplements
Fish oil and other omega-3 supplements have mild blood-thinning properties. Combining them with other supplements that affect clotting—such as high-dose vitamin E, ginkgo biloba, or garlic supplements—may have additive effects. Individually, these effects are usually modest, but combining multiple blood-thinning supplements could potentially increase bleeding risk, particularly before surgery.
⚠️ Important: If you’re scheduled for surgery, inform your healthcare team about all supplements you take. Many surgeons recommend stopping fish oil, vitamin E, and certain herbal supplements one to two weeks before procedures due to potential bleeding concerns.

Supplement and Medication Interactions
Interactions between supplements and prescription medications deserve particular attention because the consequences can be more serious. If you take any regular medication, this section is especially relevant.
Blood Thinners (Anticoagulants)
Warfarin and other vitamin K antagonists are among the medications most affected by supplements. Vitamin K directly counteracts warfarin’s mechanism of action. Sudden increases or decreases in vitamin K intake—whether from food or supplements—can destabilise INR (a measure of blood clotting) and either increase bleeding risk or reduce the medication’s protective effect.
Beyond vitamin K, supplements with blood-thinning properties can amplify anticoagulant effects. Fish oil, vitamin E, ginkgo, garlic, ginger, and turmeric have all been flagged as potentially increasing bleeding risk when combined with anticoagulants. If you take warfarin or similar medications, discuss any supplement changes with your anticoagulation clinic.
Thyroid Medications
Levothyroxine (thyroid hormone replacement) is sensitive to numerous supplement interactions. Calcium, iron, magnesium, and zinc can all bind to levothyroxine in the gut, reducing its absorption. Soy isoflavones may also interfere with thyroid hormone activity.
The standard advice is to take levothyroxine on an empty stomach, ideally first thing in the morning, and wait at least four hours before taking mineral supplements. Coffee can also reduce levothyroxine absorption, so water is the recommended beverage.
Medications Affected by St John’s Wort
St John’s Wort induces cytochrome P450 enzymes, particularly CYP3A4, which metabolises a remarkably long list of medications. Affected drugs include:
- Oral contraceptives (reduced effectiveness, risk of unplanned pregnancy)
- Immunosuppressants (organ rejection risk in transplant patients)
- HIV medications (reduced viral suppression)
- Some cancer treatments (reduced effectiveness)
- Certain antidepressants (risk of serotonin syndrome)
- Anticoagulants (altered blood thinning effect)
Given the breadth of potential interactions, many healthcare professionals advise against St John’s Wort for anyone taking regular medications. If you’re considering it for low mood, discuss alternatives with your GP.
Diabetes Medications
Several supplements may affect blood sugar levels, which can be problematic if you take diabetes medications. Chromium, berberine, cinnamon, and alpha-lipoic acid have all been studied for blood sugar effects. Whilst some people with diabetes use these supplements therapeutically (under medical supervision), combining them with glucose-lowering medications without adjustment could theoretically increase hypoglycaemia risk.
Blood Pressure Medications
Potassium supplements require caution if you take ACE inhibitors or potassium-sparing diuretics, as these medications can already elevate potassium levels. Excessive potassium (hyperkalaemia) can cause dangerous heart rhythm disturbances. Conversely, some supplements like liquorice root can raise blood pressure and counteract antihypertensive medications.
| Medication Type | Supplements Requiring Caution | Potential Concern |
|---|---|---|
| Warfarin/Anticoagulants | Vitamin K, fish oil, vitamin E, ginkgo, garlic | Altered clotting, bleeding risk |
| Levothyroxine | Calcium, iron, magnesium, zinc, soy | Reduced medication absorption |
| Antidepressants (SSRIs) | St John’s Wort, 5-HTP, SAMe | Serotonin syndrome risk |
| ACE Inhibitors | Potassium supplements | Hyperkalaemia risk |
| Diabetes medications | Chromium, berberine, alpha-lipoic acid | Hypoglycaemia risk |
| Immunosuppressants | St John’s Wort, echinacea | Altered drug levels, rejection risk |
Nutrient Absorption Conflicts
Understanding how nutrients compete for absorption can help you make smarter decisions about when and how to take your supplements.
Fat-Soluble Vitamins
Vitamins A, D, E, and K all require dietary fat for optimal absorption. Taking these supplements with a meal containing some fat—olive oil, avocado, nuts, or even just butter on toast—may improve how well your body absorbs them.
There’s some theoretical concern that very high doses of one fat-soluble vitamin might compete with others for absorption, though this is less well-documented than mineral competition. Taking a balanced approach rather than mega-dosing individual fat-soluble vitamins is generally advisable.
The Mineral Competition Problem
Divalent minerals—those with a +2 charge, including calcium, magnesium, iron, zinc, and copper—tend to compete most directly with each other. They often use similar transport proteins (like DMT1) to cross the intestinal wall. When multiple competing minerals are present simultaneously, absorption of each may be reduced.
The practical implication: if you take multiple mineral supplements, consider spacing them throughout the day rather than taking everything at once. This allows each mineral a better opportunity to absorb without competition.
Fibre and Mineral Binding
High-fibre foods and fibre supplements can bind certain minerals, reducing their absorption. Phytic acid in whole grains and bran is particularly notable for binding iron, zinc, and calcium. This doesn’t mean you should avoid fibre—its benefits for digestive health and blood sugar regulation are well-established. However, taking mineral supplements separately from high-fibre meals or fibre supplements might improve absorption.
Tannins and Polyphenols
Tea, coffee, and red wine contain compounds that can inhibit iron absorption. If you’re taking iron supplements to address deficiency, consuming them with plain water rather than tea or coffee is advisable. Waiting an hour or so after taking iron before drinking these beverages may help.
💡 Tip: Vitamin C may enhance iron absorption from supplements, particularly non-heme iron (the form found in most supplements). Taking iron with a glass of orange juice or a vitamin C supplement could be beneficial if you’re trying to improve iron status.
Safe Supplement Timing Strategies
One of the most practical ways to manage supplement interactions is through strategic timing. Here’s a framework for thinking about when to take different supplements.
Morning (With Breakfast)
B vitamins are often taken in the morning because some people find them mildly energising—taking them late in the day might affect sleep for sensitive individuals. Fat-soluble vitamins (A, D, E, K) benefit from being taken with a meal containing fat, and breakfast often fits this requirement.
If you take thyroid medication, this should generally come first, ideally 30-60 minutes before breakfast and supplements, taken with water only.
Midday (With Lunch)
If you need to separate competing minerals, lunch provides a convenient second dosing window. For example, if you take calcium with breakfast, iron might be better suited to lunchtime (or vice versa). This separation may help optimise absorption of both.
Evening (With Dinner or Before Bed)
Magnesium is commonly taken in the evening due to its potential relaxation and sleep-supporting properties. Calcium and vitamin D can also be taken with dinner if that’s more convenient for your routine.
Fish oil and other omega-3 supplements are often tolerated better with larger meals, which can reduce any fishy aftertaste or digestive upset.
Sample Timing Schedule
| Time | Supplements | Rationale |
|---|---|---|
| Early morning (empty stomach) | Thyroid medication (if applicable) | Optimal absorption without interference |
| Breakfast (with fat) | Multivitamin, vitamin D, B vitamins | Fat aids absorption; B vitamins taken early |
| Lunch (with food) | Iron (with vitamin C), zinc | Separated from calcium; vitamin C enhances iron |
| Dinner (with food) | Calcium, fish oil, CoQ10 | Separated from iron/zinc; larger meal aids tolerance |
| Before bed | Magnesium glycinate | Relaxation benefits; separated from other minerals |
This is a general framework—your optimal schedule depends on which supplements you take, your medication regimen, and your lifestyle. Some flexibility is fine; the goal is to avoid taking directly competing supplements at exactly the same time, not to achieve perfect precision.
High-Risk Combinations to Avoid
Whilst many supplement interactions are manageable through timing or dose adjustment, some combinations warrant particular caution or should generally be avoided without medical supervision.
Multiple Blood-Thinning Supplements
Combining several supplements that affect blood clotting—fish oil, vitamin E, ginkgo biloba, garlic, ginger, turmeric, nattokinase—may additively increase bleeding risk. Taking one of these is usually fine for most people, but stacking multiple blood-thinning supplements should prompt a conversation with your healthcare provider, especially if you have any bleeding disorder or take anticoagulant medications.
St John’s Wort With Almost Any Medication
Given its wide-ranging effects on drug metabolism, St John’s Wort should generally be avoided if you take prescription medications. The potential for reducing medication effectiveness—sometimes with serious consequences—makes this herbal supplement high-risk for many people.
High-Dose Vitamin A and Retinoid Medications
Prescription retinoids (like isotretinoin for acne) are vitamin A derivatives. Taking high-dose vitamin A supplements alongside these medications could potentially lead to vitamin A toxicity. If you’re on retinoid therapy, discuss vitamin A intake with your prescriber.
Multiple Stimulating Supplements
Combining caffeine-containing supplements with other stimulants like ephedra (now banned in the UK), bitter orange, or excessive green tea extract may increase cardiovascular strain. Heart palpitations, anxiety, and elevated blood pressure are potential concerns.
High-Dose Single Nutrients Over Extended Periods
Mega-dosing individual nutrients can create imbalances. High-dose zinc depleting copper, excessive vitamin B6 causing nerve damage, and prolonged high-dose vitamin A causing toxicity are all documented concerns. Following recommended doses and taking breaks from high-dose protocols (when used therapeutically) is generally advisable.
🚨 Warning: If you experience unexpected symptoms after starting a new supplement—particularly bruising, bleeding, heart palpitations, severe digestive upset, or neurological symptoms—stop the supplement and consult a healthcare professional promptly.

How to Research Your Own Supplements
Empowering yourself with reliable information helps you have better conversations with healthcare providers and make more informed decisions.
Reliable Interaction Checkers
Several online tools can help you identify potential interactions:
- Drugs.com Interaction Checker: Includes many supplements alongside medications
- WebMD Interaction Checker: Another comprehensive tool covering supplements
- Natural Medicines Database: The most comprehensive resource, though full access requires subscription (some healthcare providers have access)
These tools are helpful starting points, but they have limitations. They may flag theoretical interactions that aren’t clinically significant, or miss newer supplements without established data. Use them as one input alongside professional advice.
Reading Product Labels Carefully
Quality supplement brands often include interaction warnings on their labels or package inserts. Check for statements like “do not use if taking blood thinners” or “consult a healthcare professional if taking prescription medications.” These warnings, whilst sometimes broad, indicate the manufacturer has considered interaction potential.
Evidence-Based Resources
For deeper research into specific supplements, consider:
- NIH ODS — Fact Sheets – Comprehensive information on vitamins and minerals
- Examine — Supplement Interactions – Evidence summaries with interaction information
- PubMed — Supplement Drug Interactions – Original research studies (though often technical)
Keeping Records
Maintain a simple list of all supplements and medications you take, including doses and timing. This makes it easier to discuss your regimen with healthcare providers, check for interactions, and track any changes. Some people find apps like MyFitnessPal or specialised medication trackers helpful for this purpose.
Working With Healthcare Professionals
Navigating supplement interactions doesn’t have to be a solo endeavour. Healthcare professionals can provide valuable guidance, though you may need to initiate the conversation.
Your GP
GPs can help identify potential interactions with your medications and may suggest blood tests to monitor relevant markers (like vitamin D levels or iron status). However, many GPs have limited time and training specifically in supplements, so coming prepared with specific questions helps. Asking “Could this supplement interact with my medications?” is more productive than a vague “What supplements should I take?”
Pharmacists
Pharmacists are often underutilised resources for interaction checking. They have access to comprehensive databases and are trained to identify drug interactions—many of which extend to supplements. Community pharmacists can often review your supplement and medication list and flag concerns. This service is typically free and doesn’t require an appointment.
Registered Dietitians
For nutrition-specific guidance, registered dietitians (look for RD or RNutr credentials) have extensive training in nutrient interactions and can help you develop a coherent supplementation strategy that complements your diet. They may be available through the NHS for certain conditions, or privately.
Clinical Pharmacologists
For complex medication regimens with multiple potential interactions, a clinical pharmacologist consultation (usually via referral) can provide specialist input. This is particularly relevant for people taking many medications alongside supplements.
✓ Key Takeaways
- Bring a complete list of supplements and medications to appointments
- Ask specifically about interactions when starting new supplements
- Pharmacists are accessible, knowledgeable resources for interaction checking
- Don’t assume “natural” means “no interactions”—many herbal products interact significantly
- Report any new symptoms after starting supplements to your healthcare provider
Safety Considerations and Precautions
Before we move to frequently asked questions, let’s consolidate the key safety points everyone should keep in mind.
Who Needs Extra Caution
Certain groups should be particularly careful about supplement interactions:
- People taking prescription medications: Especially anticoagulants, thyroid medications, immunosuppressants, or psychiatric medications
- Those with chronic health conditions: Kidney disease, liver disease, and bleeding disorders all affect how supplements are processed and tolerated
- Pregnant or breastfeeding women: Some supplements are beneficial, others potentially harmful—professional guidance is essential
- People scheduled for surgery: Many supplements should be stopped one to two weeks before procedures
- Older adults: Polypharmacy (multiple medications) increases interaction risk; kidney and liver function changes may affect supplement processing
Warning Signs to Watch For
Be alert to symptoms that might indicate a problematic interaction:
- Unusual bruising or bleeding
- Digestive upset that persists beyond initial adjustment
- Mood changes, particularly with supplements affecting brain chemistry
- Heart palpitations or blood pressure changes
- Symptoms that worsen conditions you’re treating with medication
- New symptoms coinciding with supplement changes
The “More Is Better” Fallacy
Higher doses don’t necessarily provide greater benefits, and they do increase interaction and toxicity risks. Fat-soluble vitamins (A, D, E, K) accumulate in body tissues, meaning excessive intake can lead to toxicity over time. Even water-soluble vitamins and minerals can cause problems at very high doses. Following recommended serving sizes and using high-dose protocols only under professional supervision is prudent.
Quality Matters
Supplements from reputable manufacturers are more likely to contain what they claim and be free from contaminants. Look for third-party testing certifications and be wary of products with outlandish claims or suspiciously low prices. Contaminated or mislabelled supplements add unpredictable variables to any interaction considerations.
Recommended Products
Daily Supplement Organiser with Timer Caps
A practical solution for managing complex supplement routines, helping you time doses correctly and avoid taking competing supplements together.
- Seven-day organiser with AM/PM compartments
- Timer caps show hours since last opened
- Compact design for home or travel use
Balanced Daily Multivitamin Complex
A comprehensive formula designed with balanced ratios to minimise competition between nutrients, providing broad nutritional support in a single daily dose.
- Balanced mineral ratios (includes copper with zinc)
- Active B vitamin forms for optimal utilisation
- Gentle iron form less likely to cause digestive upset
Frequently Asked Questions
Can I take all my supplements at the same time?
Whilst convenient, taking all supplements together isn’t always optimal. Minerals like calcium, iron, and zinc compete for absorption when consumed simultaneously. Fat-soluble vitamins need dietary fat for best absorption. A better approach is grouping supplements strategically—for example, fat-soluble vitamins with breakfast, iron at lunch (away from calcium), and magnesium in the evening. That said, for people with simpler routines taking modest doses, timing is less critical than actually remembering to take them consistently.
How do I know if my supplements are interacting with my medication?
Signs might include your medication becoming less effective (condition symptoms returning), unexpected side effects, or new symptoms coinciding with supplement changes. However, many interactions don’t cause obvious symptoms—they simply alter drug levels in ways that may not be immediately apparent. The safest approach is checking for interactions before starting new supplements, ideally with a pharmacist review, rather than waiting to notice problems.
Are herbal supplements safer than vitamin and mineral supplements?
Not necessarily. Herbal supplements often contain complex mixtures of active compounds that can interact with medications in significant ways. St John’s Wort is a prime example—it affects the metabolism of numerous prescription drugs. “Natural” doesn’t mean “interaction-free.” Many potent pharmaceutical drugs are derived from plants, after all. Herbal supplements deserve the same careful interaction checking as any other supplement.
Should I stop all supplements before surgery?
Many surgeons recommend stopping supplements that affect blood clotting—including fish oil, vitamin E, garlic, ginkgo, and turmeric—one to two weeks before surgery. Other supplements may also need to be paused depending on the procedure. Always disclose your full supplement list to your surgical team; they can provide specific guidance based on your procedure and individual circumstances.
Can supplement interactions cause permanent harm?
Most supplement interactions cause temporary effects that resolve once the problematic combination is stopped. However, some situations can cause serious harm—for example, St John’s Wort reducing immunosuppressant levels could lead to organ rejection in transplant patients, or combined blood thinners causing dangerous bleeding. Interactions affecting medication for life-threatening conditions are the highest-risk scenarios. This is why checking for interactions before starting supplements, particularly if you take prescription medications, is so important.
Do I need to worry about food-supplement interactions too?
Yes, food can affect supplement absorption and effectiveness. Calcium from dairy can reduce iron absorption; caffeine and tannins in tea inhibit iron; high-fibre meals can bind minerals; grapefruit affects the metabolism of various substances. These interactions are generally less dramatic than supplement-drug interactions but can be relevant if you’re taking supplements to address specific deficiencies. Following guidance like “take iron on an empty stomach” or “take with food containing fat” accounts for these interactions.
Final Thoughts
Understanding supplement interactions empowers you to make smarter decisions about your health routine. The goal isn’t to become anxious about every possible interaction, but rather to approach supplementation thoughtfully—considering timing, being aware of the most significant interactions, and communicating openly with healthcare providers.
For most people, a few simple strategies make a meaningful difference: separating competing minerals by a few hours, taking fat-soluble vitamins with meals, and checking for interactions before starting new supplements when taking prescription medications. These practices don’t require perfection, just reasonable attention.
Remember that supplements are one part of a broader health picture. They work best when combined with a varied diet, adequate sleep, regular movement, and appropriate medical care. When interactions concern you, pharmacists offer an accessible, knowledgeable resource for checking compatibility—often more conveniently than waiting for a GP appointment.
If you found this guide helpful, you might also explore our vitamin B1 essential guide for detailed information on that specific nutrient. Building your knowledge one topic at a time helps you become a more informed participant in your own health decisions.
Sources
- NHS. “Vitamins and Minerals.” NHS Choices. NHS — Supplement Interactions
- National Institutes of Health. “Dietary Supplement Fact Sheets.” NIH Office of Dietary Supplements. NIH ODS — All Fact Sheets
- Stargrove MB, et al. “Herb, Nutrient, and Drug Interactions: Clinical Implications.” Mosby Elsevier. PubMed — Drug Interactions
- Mayo Clinic Staff. “Dietary Supplements: What You Need to Know.” Mayo Clinic. Mayo Clinic — Supplement Interactions
- Harvard Health Publishing. “Supplements and Safety.” Harvard Medical School. Harvard Health — Supplement Safety
- Cleveland Clinic. “Vitamins & Supplements: Interactions and Guidelines.” Cleveland Clinic Health Library. Cleveland Clinic — Vitamin Interactions
- Examine.com. “Supplement Interaction Research.” Examine. Examine — Supplement Interactions
Written by Arsim Rama
Health Content Specialist · Last reviewed: January 2026
Affiliate Disclosure: This article may contain affiliate links. If you purchase through these links, we may earn a small commission at no extra cost to you. We only recommend products we believe in.
Medical Disclaimer: This article is for educational purposes only and does not constitute medical advice. Always consult your GP or a qualified healthcare professional before making changes to your supplement routine, especially if you take prescription medications.