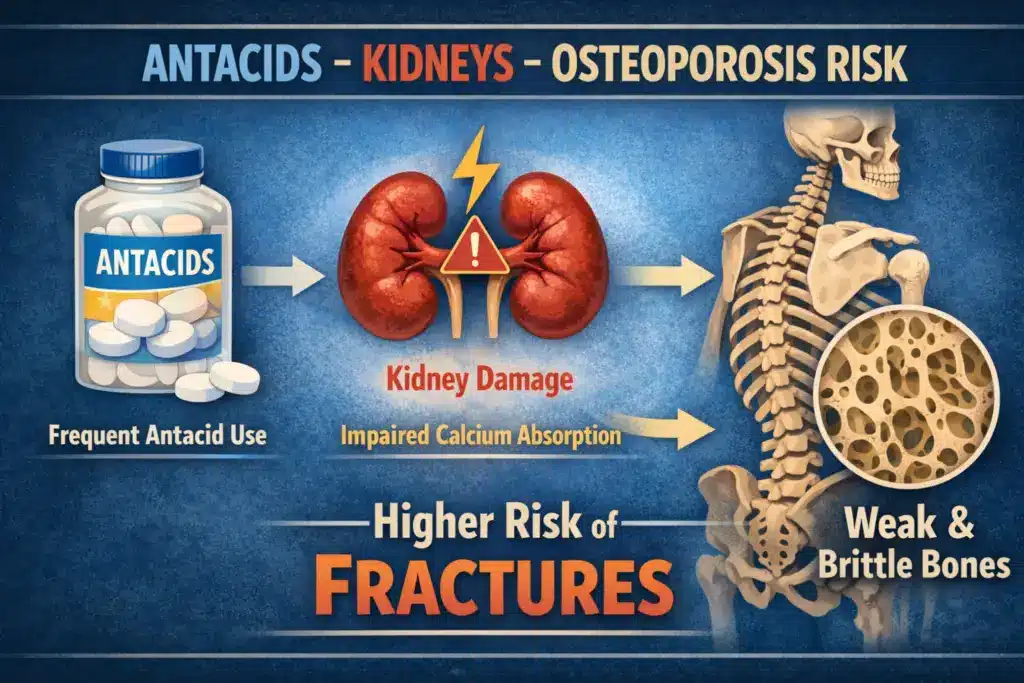
Quick Answer: Antacids can affect the kidneys in certain situations, especially with high doses, long-term use, or existing kidney disease. Some acid-suppressing medicines (particularly long-term PPIs) are also linked with a small increase in fracture risk in observational research. The practical takeaway: match the product to your symptoms, avoid chronic self-dosing, and get your GP involved if you need frequent relief.
Do antacids affect kidneys and increase osteoporosis risk? They can, mainly when used often or in high doses, or when someone has chronic kidney disease. Calcium-based antacids may cause high calcium in rare cases, while long-term acid suppression can affect mineral absorption. Safer use starts with correct dosing and medical review.
Imagine you’re reaching for antacids most evenings after dinner. The burning settles, you get on with your night, and it feels harmless because it’s over-the-counter. Then you see a headline about kidney damage and osteoporosis and think, “Hang on… is this something I should worry about?”
This guide unpacks what the research suggests, what’s still uncertain, and how to make sensible choices if you need heartburn relief. We’ll compare common antacid ingredients, explain why certain people are more vulnerable (including those with kidney disease), and look at the osteoporosis question without panic. If you also use supplements, you may find our iron supplements guide helpful, because acid reducers and minerals often interact in surprising ways.
Evidence Snapshot
Long-term PPI use is associated with a modest increase in fracture risk in observational studiesModerateThe increase is small; causation isn’t proven. Best practice is “lowest effective dose, shortest necessary time”.Certain antacid ingredients can accumulate in kidney disease (e.g., magnesium or aluminium)StrongIf you have CKD, ingredient choice matters and should be checked with a clinician.
☑️ Key Takeaways
- “Antacid” can mean different things: simple neutralisers (like calcium carbonate) aren’t the same as PPIs or H2 blockers.
- Kidney risk is most relevant with heavy use, dehydration, older age, and especially chronic kidney disease.
- Bone concerns are more often discussed with long-term acid suppression (not just occasional chewable antacids).
- Persistent symptoms need a plan, not endless OTC dosing. A GP review is the safest shortcut.
What counts as an “antacid” (and what doesn’t)
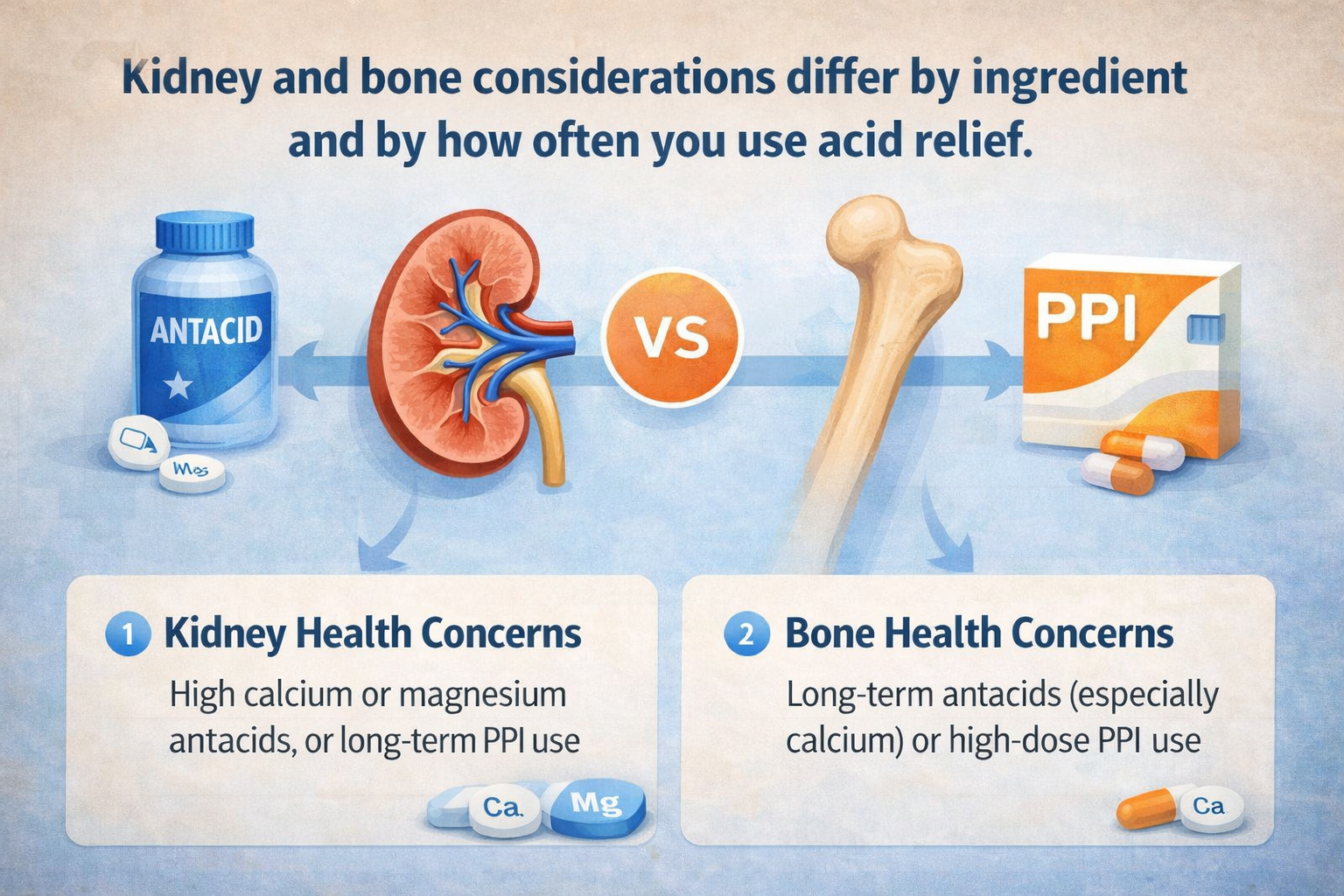
People often say “antacids” when they mean any heartburn medicine. In practice, there are three common groups, and their kidney and bone considerations differ:
- Antacids (neutralizers): Work quickly by neutralizing stomach acid. Common ingredients include calcium carbonate, magnesium hydroxide, aluminium hydroxide, and sodium bicarbonate.
- H2 blockers (acid reducers): Reduce acid production for several hours (e.g., famotidine). Not an “antacid” in the strict sense, but often used for the same symptoms.
- PPIs (strong acid suppression): Reduce acid production more powerfully (e.g., omeprazole, lansoprazole). Usually taken daily for a course, not “as needed”.
🧠 Tip: If you need “something” most days, it’s worth identifying which bucket you’re in. Ongoing daily symptoms are a signal to review triggers, timing, and diagnosis, not just switch brands.
How antacids can affect the kidneys (the short version)
Here’s the surprising part: the kidney concern usually isn’t from one normal dose. It’s from the pattern. The kidneys act like your body’s filter and balancing system. If you pour too much of a mineral or alkali into the system, the filter has to keep up. When it can’t (or when it’s already under strain), problems are more likely.
Think of it like a sponge absorbing water. A sponge can cope with a spill. But if you keep pouring, and the sponge is already partly soaked (age, dehydration, kidney disease), it stops coping and the overflow shows up elsewhere.
Why occasional use is different from chronic exposure
Most kidney concerns sit in the gap between a single dose and a long-running habit. One normal dose of an antacid is usually handled without drama, because healthy kidneys are good at maintaining acid–base balance and keeping minerals in a safe range. The problem is that frequent dosing can gradually shift the “background conditions” your kidneys are working in, especially if you’re also dehydrated, older, or living with chronic kidney disease (CKD).
Here’s what your kidneys are doing in the background. They help regulate the body’s pH by controlling how much bicarbonate is kept or excreted, and they fine-tune minerals like calcium, magnesium, sodium, and phosphate. When you take certain antacids repeatedly, you’re not only neutralising acid in the stomach. You may also be adding extra minerals (like calcium or magnesium) and extra “alkali” load (substances that can raise pH) that the kidneys need to process.
For someone with healthy kidney function, this is often manageable, especially at label doses. But if kidney function is reduced, the clearance of certain minerals can slow down. That’s why magnesium- and aluminium-containing antacids are more concerning in CKD: the risk is less about the stomach and more about accumulation over time.
🧠 Tip: If you’re using antacids most days, treat it like a “recurring symptom” rather than a quick fix. Track frequency for two weeks. That simple data point helps a GP or pharmacist decide whether you need an ingredient change, a short course of a different medicine, or an investigation of the cause.
It also helps to separate two ideas people often mix up: acute kidney injury versus chronic kidney strain. Acute kidney injury is a sudden drop in kidney function, sometimes triggered by dehydration, illness, or rare metabolic imbalances. Chronic strain is slower and often silent, where the kidneys have less “buffer” for extra loads. Heavy antacid use doesn’t automatically cause either, but it can become one piece of a larger picture when other risk factors are present.
1) Calcium carbonate: when “bone-friendly” becomes too much
Calcium carbonate antacids are popular because they work fast and are widely available. The main kidney-related risk with heavy use is high blood calcium, especially when combined with other calcium supplements or vitamin D, and when fluid intake is low. In more severe cases, the combination of high calcium and absorbable alkali can contribute to acute kidney injury.
⏰ Caution: If you use calcium carbonate antacids daily and you also take calcium supplements for bone health, it’s worth checking your total intake with a clinician. “More” isn’t always better, especially if your kidneys are not at full strength.
2) Magnesium-containing antacids: fine for many, risky in CKD
Magnesium hydroxide can help neutralise acid and also acts as an osmotic laxative in some products. In healthy kidneys, excess magnesium is usually excreted. With chronic kidney disease, magnesium can build up more easily. That’s why clinicians often advise people with CKD to avoid magnesium-containing antacids unless specifically approved.
3) Aluminium-containing antacids: the “avoid in CKD” classic
Aluminium hydroxide antacids are less common than they used to be, but they still exist. Aluminium is a bigger concern when kidney function is reduced because the body can’t clear it well. For people with significant CKD (and especially those on dialysis), this is one of the ingredients that clinicians tend to steer away from due to accumulation risk.
4) Sodium bicarbonate and high sodium loads
Some products contain sodium bicarbonate (bicarbonate of soda). Bicarbonate can neutralise acid, but sodium load can be an issue for people with high blood pressure, heart failure, or kidney disease. It’s not automatically “bad”, but it’s not the best default for frequent use if sodium is a concern.
Who is most at risk (and who usually isn’t)
For most healthy adults using antacids occasionally, the kidney risk is low. The risk rises when the same pattern shows up again and again: higher dose, longer duration, and less physiological “buffer”.
- Chronic kidney disease (any stage): Ingredient choice matters. Magnesium and aluminium are the usual red flags.
- Older adults: Kidney function typically declines with age, even without a formal CKD diagnosis.
- Dehydration or frequent vomiting/diarrhoea: Fluid and electrolyte shifts make “mineral-heavy” products riskier.
- People taking multiple supplements: Calcium + vitamin D + calcium carbonate antacids can stack up.
- People using daily acid suppression long-term: That’s where bone questions are more often raised.
📢 Warning: Seek medical advice promptly if you have heartburn plus trouble swallowing, unexplained weight loss, vomiting blood, black stools, persistent vomiting, or chest pain. Those symptoms need assessment and aren’t for self-treatment.
Do antacids increase osteoporosis risk?
The osteoporosis conversation is often muddled because different medicines get lumped together. Occasional neutralising antacids (like a few chewables per week) are not the main focus of fracture-risk discussions. The concern is more often raised around long-term acid suppression, especially with PPIs, and sometimes around chronic high-dose use patterns.
Why might this matter? Acid helps with the absorption of some minerals and nutrients. Lowering stomach acid long-term may change absorption patterns, and it may influence magnesium levels in some people. That doesn’t mean “PPIs cause osteoporosis” in a straight line, but research has repeatedly found a modest association between long-term PPI use and fracture risk. Association isn’t the same as cause, and people who need PPIs often have other risk factors as well.
A practical way to think about it is like watering plants: the aim isn’t to stop watering, it’s to water appropriately. If you need a PPI for a diagnosed condition, the goal is to use it correctly and review it periodically, while also supporting bone health with basics that matter more (protein intake, resistance training, vitamin D status, and total calcium intake from food).
Antacids, PPIs, and bone health: what actually happens in the body
When people worry about osteoporosis risk from heartburn medicines, they often imagine acid as something you simply “turn off”. In reality, stomach acid is part of digestion’s normal workflow. It helps break down food, and it can influence how well certain nutrients dissolve and become available for absorption. This is one reason long-term acid suppression (particularly with PPIs) gets more attention than the occasional chewable antacid.
Mineral absorption: solubility matters
Calcium is a useful example. Calcium carbonate needs a more acidic environment to dissolve well, so it tends to absorb best with meals and may be more sensitive to low stomach acid. Calcium citrate dissolves more easily and is often better tolerated across a wider range of stomach acidity. This doesn’t mean one is “good” and the other is “bad”, but it explains why the form matters when you’re thinking about long-term patterns and bone support.
Magnesium is another mineral that sits at the crossroads of bone and muscle function. Most people meet their needs through diet, but some long-term medicine patterns are associated with lower magnesium in certain individuals. If you’re on long-term acid suppression and you have symptoms that could fit low magnesium (like persistent muscle cramps or unusual fatigue), it’s worth asking your clinician whether testing is appropriate rather than self-prescribing high doses.
Why fracture risk is not the same as osteoporosis
It’s also important to separate fracture risk from osteoporosis. Osteoporosis is a condition of reduced bone density and quality. Fracture risk is broader: it includes bone strength, yes, but also balance, muscle mass, vision, medication side effects, and fall risk. Observational research linking long-term PPI use to fractures may reflect multiple factors, including the health profile of people who need PPIs in the first place.
In practical terms, if bone health is your concern, the biggest “needle movers” are usually not the antacid itself. They are consistent strength training, adequate protein, avoiding smoking, moderating alcohol, and keeping vitamin D status in a healthy range. Medicines sit on top of those foundations. If you’re using a PPI long-term, a regular review with your GP can help confirm you still need it and whether a step-down plan is safe.
⏰ Important: Don’t stop prescribed acid-suppressing medicines abruptly without advice, especially if you’ve been on them for months. Rebound symptoms are common, and a structured step-down is often more comfortable and sustainable.
Synergy Table: habits that support relief + bone health
Synergy Types: 🔄 Absorption | ⚡ Activation | 🛡️ Protection | 🔗 Cofactor | ⏱️ Timing
Evidence: ⭐⭐⭐ Strong | ⭐⭐ Moderate | ⭐ Emerging
Comparison: antacids vs H2 blockers vs PPIs (kidney & bone)
If you’re worried, the goal is not to find a “perfect” product. It’s to match the tool to the job and avoid long-term self-treatment. In a way, these medicines are like dance partners: the right match feels smooth; the wrong match keeps stepping on toes.
A practical, kidney- and bone-aware heartburn plan
If you’ve been taking something regularly, this is the part that often helps most: a simple plan that reduces the need for constant dosing.
Step 1: decide if this is “occasional” or “frequent”
- Occasional: A few times a month, tied to obvious triggers.
- Frequent: Most weeks, or several days per week, or it’s waking you at night.
Frequent symptoms are where risks and missed diagnoses become more relevant. It’s also where non-medicine changes can make the biggest dent.
Step 2: fix the high-impact triggers first
- Large late meals (portion size often matters more than specific foods)
- Alcohol close to bedtime
- Very fatty meals that sit longer in the stomach
- Mint and chocolate in some people
- Eating then lying flat soon after
🧠 Tip: Try a 10-day “track and test” approach: write down what you ate, timing, and symptoms. You’re looking for repeat patterns, not perfection. This often cuts down medication use more than swapping brands.
Step 3: choose the lowest-intensity tool that works
If you rarely need relief, a simple antacid may be fine. If symptoms are frequent, talk to a pharmacist or GP about whether an H2 blocker or a short PPI course is more appropriate. The key is having an “exit plan”: step down when stable instead of continuing by habit.
If bone health is already a concern, it’s reasonable to prioritise the basics that do the heavy lifting. Consider reading our (planned) guide on vitamin D basics and comparing calcium supplement options, especially if you’re also using calcium-based antacids.
Step 4: when medication is appropriate — and when it isn’t
If you’re using an OTC product more than twice a week, it’s worth thinking in terms of “courses” and “reviews” rather than endless top-ups. For example, some people do well with an alginate product after trigger meals, because it forms a barrier without heavily changing stomach acid production. Others need an H2 blocker for predictable night symptoms. And some need a short PPI course for a defined period if GERD is confirmed or if there’s oesophageal irritation that needs time to settle.
The line you don’t want to cross is long-term self-treatment without checking the diagnosis. Persistent reflux can be driven by factors like a hiatal hernia, medication side effects, or patterns such as late meals and lying flat soon after eating. If symptoms persist despite reasonable changes, that’s a cue to involve a GP. It’s also the safest way to protect both kidneys and bones, because your clinician can account for your full history, test results, and medicine list.
🧠 Tip: If you’re taking minerals like iron, calcium, or magnesium, timing matters. As a general rule, separate antacids from mineral supplements by at least 2 hours unless your clinician advises otherwise. This simple habit can prevent “why isn’t this working?” frustration.
Product Comparison
⚠️ EDITOR: Replace #AFFILIATE-LINK-X and #PRODUCT-IMAGE-X with real URLs before publishing. Update ratings/review counts and verify UK availability.
🎥 Watch: A quick explainer on antacid types, kidney cautions, and when heartburn needs a GP review.
📜 Prefer reading? You’re already in the right place.
🏥 Expert Note
People often focus on “which antacid is safest” and miss the bigger signal: frequent heartburn is a health pattern worth checking. If you need relief most weeks, ask about the underlying driver (reflux, diet timing, medicines, H. pylori, or oesophageal irritation) so you’re not relying on indefinite self-dosing.
Safety Considerations (who should speak to a GP first)
This article is educational and can’t replace personal medical advice. If you have kidney disease, osteoporosis, take long-term medicines, or are pregnant, it’s safest to confirm your best option with a clinician. Ingredient choice and dosing can matter more than brand names.
Extra caution is sensible if you’re pregnant, older, or taking multiple long-term medicines. Pregnancy can increase reflux due to hormonal and physical changes, but ingredient choice still matters, and it’s best to confirm what’s appropriate with a midwife, GP, or pharmacist. In older adults, even mild dehydration (from low fluid intake, heat, or illness) can increase the chance of electrolyte shifts when mineral-heavy antacids are used frequently.
If you take diuretics (“water tablets”), blood pressure medicines, thyroid medication, or osteoporosis treatments, it’s also worth checking spacing and interactions. Antacids can interfere with absorption of certain medicines, and the safest strategy is often simple: avoid stacking doses close together and ask for a timing plan that fits your routine.
⏰ Important: If you need acid relief more than twice a week for several weeks, it’s a good time to speak to a GP or pharmacist. You may need evaluation (and a structured step-down plan), not stronger OTC dosing.
Frequently Asked Questions
Are chewable antacids safe if I have mild kidney disease?
It depends on the ingredient, your kidney function, and how often you use them. With CKD, magnesium – or aluminium-containing antacids are commonly avoided because reduced clearance can increase accumulation risk. Calcium-based products may be acceptable for some people, but frequent use can raise total calcium intake, especially if you also take vitamin D or calcium supplements. A pharmacist or GP can help you choose an option that fits your CKD stage, symptom pattern, and current medicines, and can advise on safer “as needed” limits.
Do PPIs cause osteoporosis, or is the risk overblown?
Long-term PPI use is linked with a modest increase in fracture risk in observational research, but that doesn’t prove PPIs directly cause osteoporosis. People who need PPIs may already have other risk factors, and fracture risk isn’t only about bone density. If you need a PPI, the safest approach is regular review, using the lowest effective dose for the shortest necessary time, and working on the foundations that protect bones: strength training, adequate protein, vitamin D status when appropriate, and avoiding smoking. If you have high fracture risk, your GP can help decide whether ongoing PPI use is still needed or whether a step-down plan is safe.
Which antacid is “best” if I’m worried about my bones?
Bone concerns are more tied to long-term acid suppression patterns than occasional neutralising antacids. If you’re using calcium carbonate frequently, the bigger issue can be total calcium intake, especially if you also supplement. If you’re on long-term PPIs, focus on whether you still need them, whether a step-down is appropriate, and the basics of bone protection. Your GP can tailor this to your risk profile.
Can antacids affect calcium absorption and make deficiency more likely?
Stomach acid plays a role in mineral absorption, but the effect varies by mineral form, dose, and the medicine used. Short-term, occasional antacid use is unlikely to cause a meaningful deficiency in a well-balanced diet. The more relevant issue is long-term daily acid suppression and overall dietary intake. If you have risk factors for low calcium or vitamin D, discuss testing and diet-first strategies.
Why do I keep needing antacids even though I’ve changed my diet?
Reflux isn’t only about “acidic foods”. Meal timing, portion size, body position after eating, alcohol, stress, certain medicines, and weight changes can all contribute. Some people also have non-acid reflux or oesophageal sensitivity, where symptoms don’t track perfectly with acid. If you’re needing frequent relief, it’s worth discussing with a clinician to confirm the driver and the best treatment path.
When should I stop self-treating and see a GP?
If symptoms are frequent (several days a week), if they’re waking you at night, or if you’ve used OTC products for weeks without improvement, a GP review is sensible. Seek urgent assessment if you have trouble swallowing, unexplained weight loss, vomiting blood, black stools, or chest pain. Those are not “wait and see” situations.
Final Thoughts
So, do antacids affect kidneys and increase osteoporosis risk? They can, but the risk is strongly shaped by dose, duration, and your health context. Occasional use is usually low risk for healthy adults. The bigger red flag is frequent reliance without a plan, especially if you have chronic kidney disease or are already concerned about bone health.
If you want a practical next step, build a simple trigger-and-timing routine and aim to reduce how often you need “rescue” products. For more day-to-day ideas, see our planned guide on everyday heartburn remedies.
Sources
- NHS — Antacids and kidney disease
- PubMed — Calcium carbonate, milk-alkali syndrome, kidney injury
- PubMed — PPIs and acute interstitial nephritis
- PubMed — PPIs and fracture risk meta-analyses
- Cleveland Clinic — Milk-alkali syndrome
- Harvard Health — PPIs and bone/fracture discussion
- NIH Office of Dietary Supplements — Fact sheets
Written by Arsim Rama
Health Content Specialist · 5+ years in nutrition research
Arsim Rama specialises in translating complex nutrition science into practical, evidence-based guidance. His work focuses on supplement safety, efficacy, and helping readers make informed health decisions.
🏥 Medically Reviewed By: Mavran Todl, Clinical Nutrition Specialist
Last medical review:
Affiliate Disclosure: This article may contain affiliate links. If you purchase through these links, we may earn a small commission at no extra cost to you. We only recommend products we genuinely believe in and have researched thoroughly.
Medical Disclaimer: This article is for educational purposes only and does not constitute medical advice. Always consult your GP or qualified healthcare professional before making changes to your health regimen, especially if you take medications or have existing health conditions.
© 2026 Paulinna. All rights reserved.